While the quality of clinical care is paramount to a patient’s health and wellbeing, patient engagement is crucial for that care to be effective. Active patient engagement can:
- Improve care outcomes
- Have a significant effect on patient satisfaction
- Reduce hospital readmissions
- Result in lower costs for both patients and health systems
Patient engagement is especially critical for successful diabetes management, in which the majority of care takes place outside of the clinician’s office or the hospital. When clinical practices offer engagement tools that improve the patient experience, it can build trust and a more positive, productive relationship between a patient and their clinician, leading to excellent health outcomes.
- Patient Engagement Strategies
- Patient Engagement Solutions for Diabetes
- How Virtual Healthcare Can Improve Patient Engagement
What is Patient Engagement?
In healthcare, “patient engagement” is an umbrella term that describes a patient’s behavioral habits when it comes to their involvement in and connection to their own care. A patient who is engaged is able to adhere to a treatment plan, retain knowledge or self-educate about their specific condition, follow their clinician’s self-management guidance, and show a willingness to maintain an ongoing dialogue with their clinician or a health coach. Engaged patients understand that their level of participation has a direct effect on their health.
The positive outcomes of treating an engaged patient are so well recognized that numerous healthcare organizational entities place engagement-related activities high in their strategic priorities. The Affordable Care Act identifies patient engagement as a quality measure in accountable care organizations (ACOs) and even mandates that these organizations make shared decision-making resources available to help integrate patient engagement into clinical practice. This provides hospitals and health systems with financial incentive to implement effective engagement strategies.
While patient participation is the key to building engagement, certain software and other digital tools can improve patients’ access to education, dedicated health coaches, and even secure, one-on-one communication with their clinicians.
How to Identify an Engaged Patient
High quality engagement comprises both the measures healthcare providers take to involve patients in their own care as well as the resulting level of patient activation. According to researcher Judith Hibbard, “patient activation” is “the measure of a patient’s understanding, competence, and willingness to participate in care decisions and processes” (via PatientEngagmentHIT).
A patient cannot successfully engage with their own care if they are not familiar with or do not fully understand their condition, associated risks, treatment options, and self-management responsibilities. In addition to providing patients with educational materials, many clinical practices use patient-facing surveys or questionnaires to determine a patient’s ability to engage. Clinicians will use the results to recommend a care program or implement the appropriate engagement strategy.
The Patient Activation Measure (PAM) is a 100-point scale that helps clinicians understand how engaged and active a patient is in their own healthcare. Survey questions are designed to assess the following in patients:
- Whether they understand the nature and causes of their health conditions
- Whether they believe they are ultimately in charge of their health
- Their ability to self-manage their conditions or treatment regimens
- Whether they know what each of their prescribed medications does
- Whether they can find solutions or communicate with their clinician when a new health issue arises
- Their ability to maintain long-term self-management of their health
- Their ability to engage in activities that maintain good health
- Their ability to participate in treatment and diagnostic choices
- Their ability to collaborate with clinicians and other providers
- Their ability to select clinicians, specialists, and provider organizations based on performance or quality
- Their ability to navigate the healthcare system
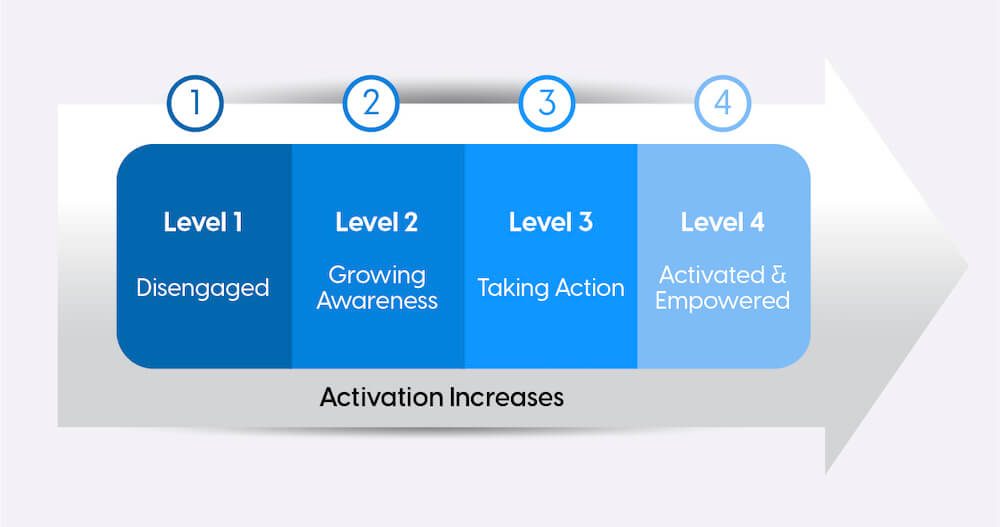
Patients are then categorized into levels of activation:
The results of a PAM survey can be integrated into electronic health records (EHR) so they remain easily accessible for clinical review.
How to Identify Non-Engaged Patients
A patient who is not actively engaged in their own health risks stalling or impeding their own progress. For example: If a patient with diabetes is not engaged with their care, they may not put effort towards understanding how a medication works and why it is important to adhere to this part of their treatment plan. Therefore, when they complete the bottle of medication, they may fail to obtain a refill, thereby risking a rise in their glucose level.
Clinicians must assess a patient’s ability to engage with their care before determining a treatment approach, especially if self-management is part of the care plan. Studies show that patients forget up to 80 percent of what their doctors tell them during appointments, so clinicians should provide their patients with supplemental information about their condition and use follow-up protocols to ensure the patient understands next steps.
Through no fault of their own, patients may experience the following barriers to successful engagement and activation:
- Technology literacy
- Language barriers
- Cognitive issues
- Lack of understanding of their health condition
- Strong allegiance to unconscious patterns of denial or dismissal
The more personalized the engagement tool or strategy, the more likely a disengaged or unmotivated patient will participate in their care. For example, a patient with low engagement and a complex self-care regimen may not be able or willing to use an app or online dashboard to manage and track their health, leading to negative health outcomes. Clinicians and health coaches can re-engage patients like this by offering them different tools and helping them set meaningful goals, such as being able to enjoy an upcoming vacation or attend a child’s sports game without health-related impediments.
Patients need the option to choose the tools and resources that will keep them most engaged; a coordinated care app may be convenient for one type of patient, whereas another may prefer regular phone calls or emails to discuss their health status.
Patient Engagement Strategies
Using their assessments of patients’ needs, preferences, and abilities, clinicians can select the engagement strategies that will be most successful for each type of patient.
Educational materials and tools
Condition-specific educational materials — including brochures, websites, or letters — can keep a patient engaged and informed between appointments, even functioning as learning activities or “homework” following a clinical visit. When choosing patient resources, clinicians should be mindful of how much a patient already knows about their condition, how much they need to know, and what is personally important to them. The results of a patient’s initial assessment will determine the complexity and volume of the resources; a more engaged patient with higher health literacy will be able to comprehend more in-depth information.
Related resource: Diabetes Patient Education: Shareable Resources for Clinicians and Patients
Choice of language and format
Resources for patients should be written in straightforward, non-medical terms in a language the patient can understand. The format of the information matters as well: some patients prefer to independently access reading materials or podcasts, whereas others may benefit from an in-person or online class led by a certified educator. One-on-one coaching can also help patients connect to and understand supplemental materials.
Shared decision-making
Patients need to feel as much a part of their care team as their clinician or care coordinator. When a patient feels included in decisions about their care, their level of engagement and activation increases. A clinician’s initial assessment should gauge a patient’s suitability to participate in shared decision-making, which includes their willingness to access educational materials, the ability to set achievable goals, and the ability to evaluate treatment options.
Multi-channel communication
Clinical practices should offer a range of communication tools for patients to choose from. Tools like apps, patient portals, automated phone calls, or supplemental care solutions can support patients outside of their clinician’s office by reminding them of upcoming appointments or alerting them to changes in their health status.
Related resource: Digital Diabetes Tools: Diabetes Prevention, Care, and Support
Ongoing assessment
Patient teach-back should be a component of every clinical interaction. Using the teach-back method, the clinician delivers information to the patient and asks them to repeat it back, thereby confirming the patient’s understanding (or lack thereof). If the patient is unable to repeat the information, the clinician can then alter their delivery. If a patient’s engagement fluctuates or declines over time, clinicians should perform another PAM assessment to determine whether they need to adjust their engagement strategy.
How Virtual Healthcare Can Improve Patient Engagement
Patients who are unable to access physical healthcare — whether due to economic barriers, lack of transportation, mental illness, or other social determinants of health — can still receive clinical guidance through virtual platforms. Patient portals, educational programs, and coordinated care solutions connect patients to experts who can recommend treatments, refer them to specialists, or even perform physical examinations with the help of a smartphone or webcam.
Provided they are tailored to the needs and abilities of the user, expert-supported virtual tools work to increase patient engagement by:
-
- Bringing health education into the patient’s home setting
- Making healthcare more convenient and less intimidating
- Reaching individuals in Health Professional Shortage Areas (HPSAs)
- Keeping all medical information in one place for ease of access
- Addressing non-medical aspects of a patient’s life, such as emotional wellbeing and social support
- Giving patients more autonomy and control over their health
When patients feel as though they are part of a team, the likelihood of positive health outcomes increases significantly. Solutions like Stability Health — which integrates clinical input, expert guidance, and personalized patient education — help foster a symbiotic relationship between the patient and all members of their care team.
Patient Engagement Solutions for Diabetes
Diabetes is a complex, sometimes unpredictable disease that requires a significant amount of self-management. Outside of the hospital or their clinician’s office, patients are primarily responsible for following their treatment plan and self-administering medication. However, the complexity of some diabetes treatment regimens can be overwhelming, frustrating, or exhausting for patients, who may become disengaged and experience a decline in health.
With the rise of mobile health, apps have become a popular tool for managing diabetes between clinical appointments. These apps provide users with a feeling of autonomy, but many operate without clinical oversight, and therefore risk negating a clinician’s recommendations or causing harm to the patient. Clinicians who wish to refer their patients to a diabetes management app must ensure that the tool contains relevant information, aligns with the patient’s health literacy level, and is easy to access and use.
The most effective tech-enabled engagement solutions for diabetes include the following:
- Personalized communication
- Secure messaging
- Expert consultation
- Medication reminders
- Appointment scheduling and reminders
- Condition-specific patient education
- Lifestyle tips
- Self-management tutorials
- Clinical coordination
- HIPAA compliance
- Mobility
- Online support or chat groups
- Live chat support
- View-download-transmit capabilities
- Pharmacy integration
Patients who have easy access to diabetes education, a dedicated health coach or nutritionist, certified diabetes educators, and expert-driven, coordinated care are more likely to stay engaged with and adhere to their treatment plan.
Stability Health is a holistic, supplemental, multi-channel solution that strives to meet individuals with complex diabetes where they are, adapting to their preferences and abilities. Each Stability Health participant has a dedicated health coach who delivers personalized, one-on-one guidance while communicating updates and recommendations to the patient’s clinician. Coaches can access a team of diabetes experts as needed to provide additional resources or clinical guidance. If a patient’s level of engagement appears to be declining, health coaches will notify the patient’s clinician and adapt their engagement strategies based on the clinician’s recommendations and assessment.
For more information about how Stability Health can best support your practice, start a conversation with our team today.